CHRONIC CARE MANAGEMENT
Help Patients Figure Out and Reach their Chronic Care Goals.
Simplify your Chronic Care Management, boost patient outcomes, and grow your revenue effortlessly—with a scalable CCM platform built to support you every step of the way.
Request a Demo

65%
CCM Enrollment
Conversion
86%
Disease-based Care
Plan Template
83%
CCM Billing from
Enrolled Patients
50%
Increase in Care
Manager Productivity
Why Wellwink’s Chronic Care Management?
The CCM platform automatically identifies eligible patients before enrollment, documents medications, calculates the total time spent with patients by tracking calls & emails, and generates invoices for guaranteed reimbursement. The system sends alerts based on the patient’s situation and the results of their monitoring device. Consequently, the providers can set the goals for their patients and keep track of their activities during the follow-up care period. Thus, the healing plan is set according to the severity of the patient’s condition.
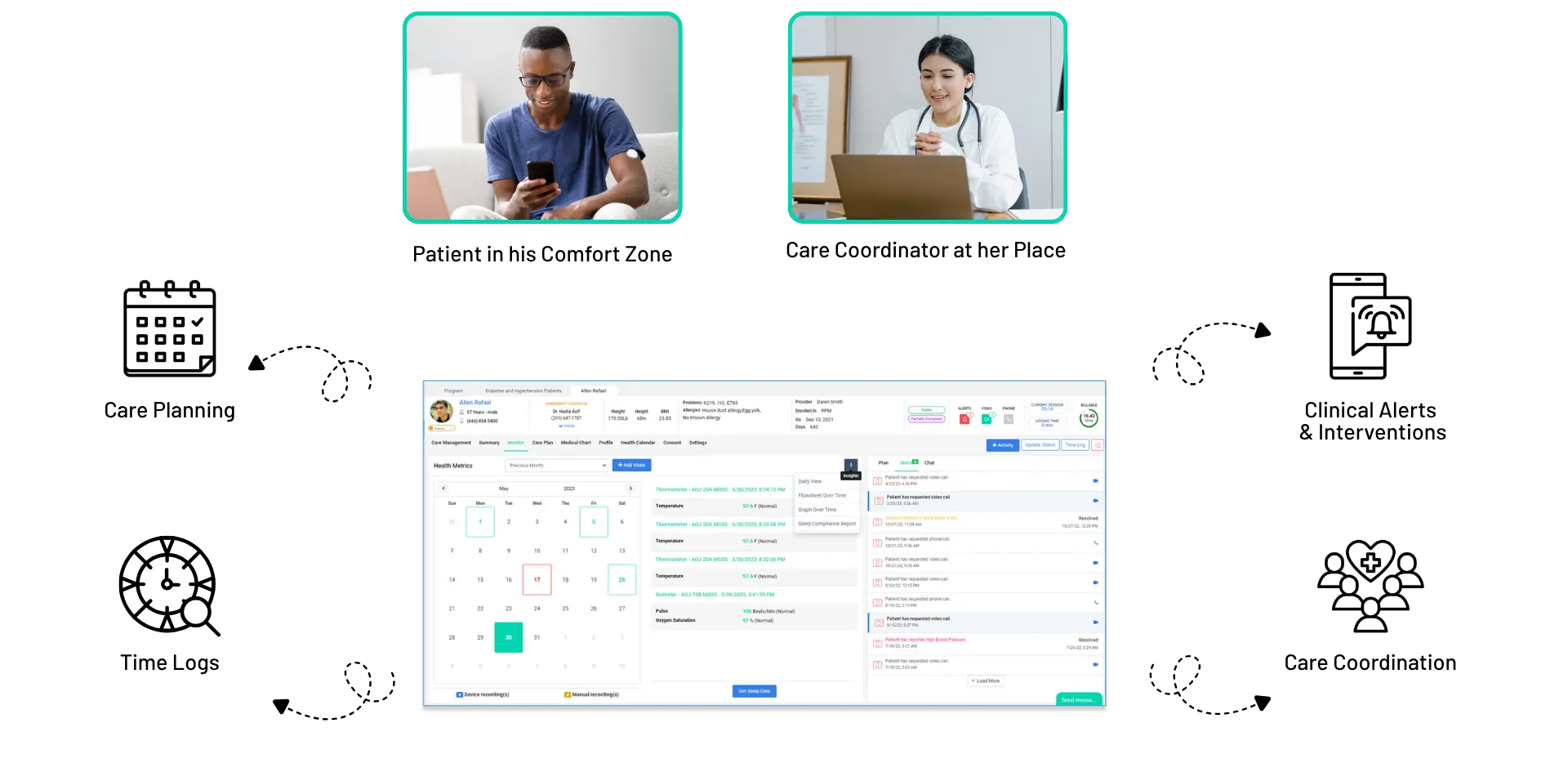
We are geared to disrupt the industry and alter the ways healthcare is provided
Request a Demo
Patients That We Enroll
Eligibility Criteria for the Patient
Life Long Patient
Insured by Medicare
2 or more chronic conditions
Not enrolled with another practitioner
- Determine if the patient meets the eligibility criteria for getting enrolled in CCM program.
- It depends on the provider to choose the diagnosed chronic conditions to bill for CCM.
- The diagnosis is expected to last for at least 12 months.
- As long as the specific requirements for the care management service type meet, there will be no limitations in the services to treat the patient.
Step-by-Step CCM System
The following diagram shows the exact flow of the CCM system.

CPT Billing Codes and Reimbursement for CCM
Non-Complex CPTs
CPT-99490
First 20 mins spent by any clinical staff or physician.
First 20 mins spent by any clinical staff or physician.
$63.43
Medicare National Payment Amount (2025)
CPT-99439
After CPT 99490, an extra 20 minutes qualifies for billing
Billable once per calendar month.
$47.83
Medicare National Payment Amount (2025)
Physician-Driven Non-Complex CPTs
CPT-99491
30 mins including first 20 mins, are spent by any clinical staff or physician
Billable once per calendar month.
$85.80
CPT-99437
30 additional minutes for provider time (no limit)
Billable once per calendar month.
$57.58
Complex CPTs
CPT-99487
60 mins are spent by any clinical staff or physician.
Billable once per calendar month.
$94.68
CPT-99489
If 30 more minutes are spent after CPT 99487, CPT 99489 can also be billed.
Billable once per calendar month.
$139.68
Request a Demo
Frequently Asked Questions
What is Chronic Care Management (CCM)?
Chronic Care Management (CCM) is a program offered by the Centers for Medicare & Medicaid Services (CMS) that provides reimbursement for non-face-to-face care management services for patients with multiple chronic conditions. The goal of CCM is to improve health outcomes, increase patient satisfaction, and reduce healthcare costs for patients with chronic conditions.
CCM services include:
- Care coordination and management – Coordinating and communicating with other healthcare providers to ensure that the patient receives appropriate care and services, and tracking the patient’s progress.
- Care planning – Developing a care plan that is tailored to the patient’s specific needs and goals, and adjusting the care plan as needed.
- Patient education and self-management support – Providing education and resources to help the patient manage their condition and promote self-management.
- Medication management – Reviewing the patient’s medications and ensuring that they are taking them correctly.
- Care transitions – Facilitating communication and coordination between the patient, family members, and caregivers, and ensuring that the patient receives appropriate care during transitions between healthcare settings.
- Follow-up and monitoring – Providing follow-up and ongoing support to help the patient maintain their health and manage their condition over time.
In order to bill for CCM services, the provider must meet certain requirements set by CMS such as:
- Patient needs to have two or more chronic conditions.
- Care plan needs to be established with the patient or their caregiver.
- Care coordination needs to be performed with other providers of the patient.
- Care needs to be provided at least 20 minutes of non-face-to-face care management services each calendar month, including care coordination and communication with other providers.
CCM services can be provided by physicians, nurse practitioners, physician assistants, nurses, and care managers.
What are the benefits of a care management program?
A care management program can provide several benefits for patients, healthcare providers, and payers:
- Improved health outcomes – Care management programs can help improve health outcomes for patients with chronic conditions by providing comprehensive, coordinated care and promoting self-management of conditions.
- Reduced healthcare costs – Care management programs can help reduce healthcare costs by avoiding unnecessary hospital readmissions and emergency department visits, and by promoting preventive care and early intervention.
- Enhanced patient satisfaction – Care management programs can enhance patient satisfaction by providing more personalized, patient-centered care, and by giving patients more control over their healthcare.
- Greater care coordination – Care management programs can promote greater care coordination among healthcare providers by facilitating communication, sharing of information, and collaboration.
- Better use of healthcare resources – Care management programs can help better use of healthcare resources by identifying and addressing gaps in care, and by promoting the most appropriate and cost-effective treatment options.
- Improved patient engagement and self-management – Care management programs can help improve patient engagement and self-management by providing education and resources, and by promoting shared decision making.
- Care continuity – Care management programs can help ensure care continuity by providing follow-up, monitoring, and tracking of patient status and health outcomes.
- Better use of technology – Care management programs can help better use of technology by implementing electronic health.
How can a chronic care management program be implemented in a medical practice?
A chronic care management program can be implemented in a medical practice by following these steps:
- Identify patients with chronic conditions – Use electronic health records (EHRs) to identify patients with chronic conditions such as diabetes, heart disease, and asthma.
- Assemble a care team – Assemble a team of healthcare professionals, including physicians, nurses, care coordinators, and other specialists, to manage the care of these patients.
- Develop a care plan – Create a personalized care plan for each patient that includes regular check-ins, lab tests, and medications.
- Utilize telemedicine – Use telemedicine to reach patients who have difficulty coming into the office, such as those who are elderly or have mobility issues.
- Monitor and track progress – Use EHRs to monitor patients’ progress and track key metrics such as blood sugar levels, blood pressure, and medication adherence.
- Coordinate with other providers – Work with other providers, such as specialists, home health agencies, and community resources, to provide comprehensive care for patients.
- Encourage self-management – Educate patients on how to manage their chronic conditions and provide resources such as educational materials and support groups.
- Measure outcomes – Regularly measure and track outcomes such as patient satisfaction, clinical outcomes, and cost savings to evaluate the success of the chronic care management program.
- Use technology – Implement technology-based solutions, such as patient engagement software, remote monitoring devices, and digital health platforms, to facilitate communication and data collection.
- Continuously evaluate and adjust – Continuously evaluate the program, gather feedback from patients, and make adjustments as needed to improve the effectiveness of the program.
What are the applicable CPT codes for CCM?
There are several Current Procedural Terminology (CPT) codes that are used to bill for chronic care management (CCM) services in the United States.
- 99487 – This code is used for the initial assessment and care planning for patients with multiple (two or more) chronic conditions that are expected to last at least 12 months, or until the death of the patient.
- 99489 – This code is used for the ongoing care management of patients with multiple (two or more) chronic conditions that are expected to last at least 12 months, or until the death of the patient.
- G0506 – This code is used for remote evaluation of recorded video and/or images furnished to the patient/caregiver.
- 99458, 99459 – These codes are used for remote evaluation of patient-transmitted recorded video or image by a physician or other qualified healthcare professional via telephone, internet, or e-mail.
It is important to note that the codes and reimbursement for CCM services may vary depending on the payer, so it’s best to check with your local Medicare administrative contractor or your private payer for more information.
What are the applicable reimbursements for CCM in 2025?
The reimbursement for chronic care management (CCM) services in 2025 will vary depending on the payer and the specific codes used to bill for the services.
For Medicare patients, the reimbursement for CCM services is as follows:
- 99487 – Initial assessment and care planning, reimbursement rate of 134.15
- 99489 – Ongoing care management, reimbursement rate of $72.23
- G0506 – Remote evaluation of recorded video and/or images, reimbursement rate of $60.81
- 99458– Used for remote physiologic monitoring, can have a reimbursement rate of approximately $38.49
- 99459 – Reimbursement Rate: a reimbursement rate of $43
It is important to note that these rates are subject to change and may vary depending on location and the specific Medicare administrative contractor.
Since the rates are not set for private payers, it’s smart to contact them for the most recent details. Payers should also inform us if any requirements, such as prior authorization, must be satisfied for reimbursement of CCM services.
It’s good to remember that CMS generally pays CCM services on a per-member-per-month (PMPM) basis. The reimbursement is decided by the number of people at the practice and not by how many patients have chronic conditions.
Resources
Wellwink Resources
Our Latest Blogs
Read the latest insights about Wellwink as well as medical blogs around the world. Our purpose is to provide education for both providers and patients.
Finding a Physician
Find a Physician and Book an Office visit or Virtual visit. We are helping healthcare communities to bridge the gap between patients and doctors.
