Advanced Primary Care Management
The Smarter Way to Manage Medicare Patients
Wellwink helps practices deliver high-quality care to every Medicare patient while ensuring transparent, timely payment — all in one easy platform.
Request a Demo

1 Month
revenue
90%
engagement and leading satisfaction ratings
$578K
1,000 patients
50%
profit margin to reinvest in your practice
Enhanced Care, Enhanced Compensation
With Wellwink, you can easily bring APCM to life — automating outreach, managing care plans, tracking engagement, and optimizing reimbursements. Wellwink enables you to scale care, stay compliant, boost revenue, and deliver better outcomes through personalized, data-driven primary care.
Designed to support value-based outcomes under fee-for-service models.
Build trusted relationships with your patients
Achieve better health outcomes for your patients
Patients are more likely to adhere to their medications and maintain healthy lifestyle habits.
CCM VS APCM
What is the difference between APCM vs. CCM?
APCM and CCM are two Medicare programs designed to reward doctors for the care they provide outside of traditional office visits. While both use a fee-for-service model to improve patient outcomes, they aren’t identical. Key differences exist regarding how each program is managed and which patients are eligible to enroll.

We help make healthcare easier for practices and more patient-focused.
Request a Demo
Patients That We Enroll
Eligibility Criteria for the APCM Patient

Patient Population
All Medicare Beneficiaries
Three Tier Model
Not enrolled with another practitioner
- Promote proactive care management for all primary care patients.
- Clinical staff under the general supervision of a billing provider.
- Includes coordination across providers and settings, medication management, and patient engagement.
- Eligibility is based on patient needs and complexity, not on time spent in care management activities.
- A patient can only be enrolled in one monthly care management program at a time.
How does APCM work?
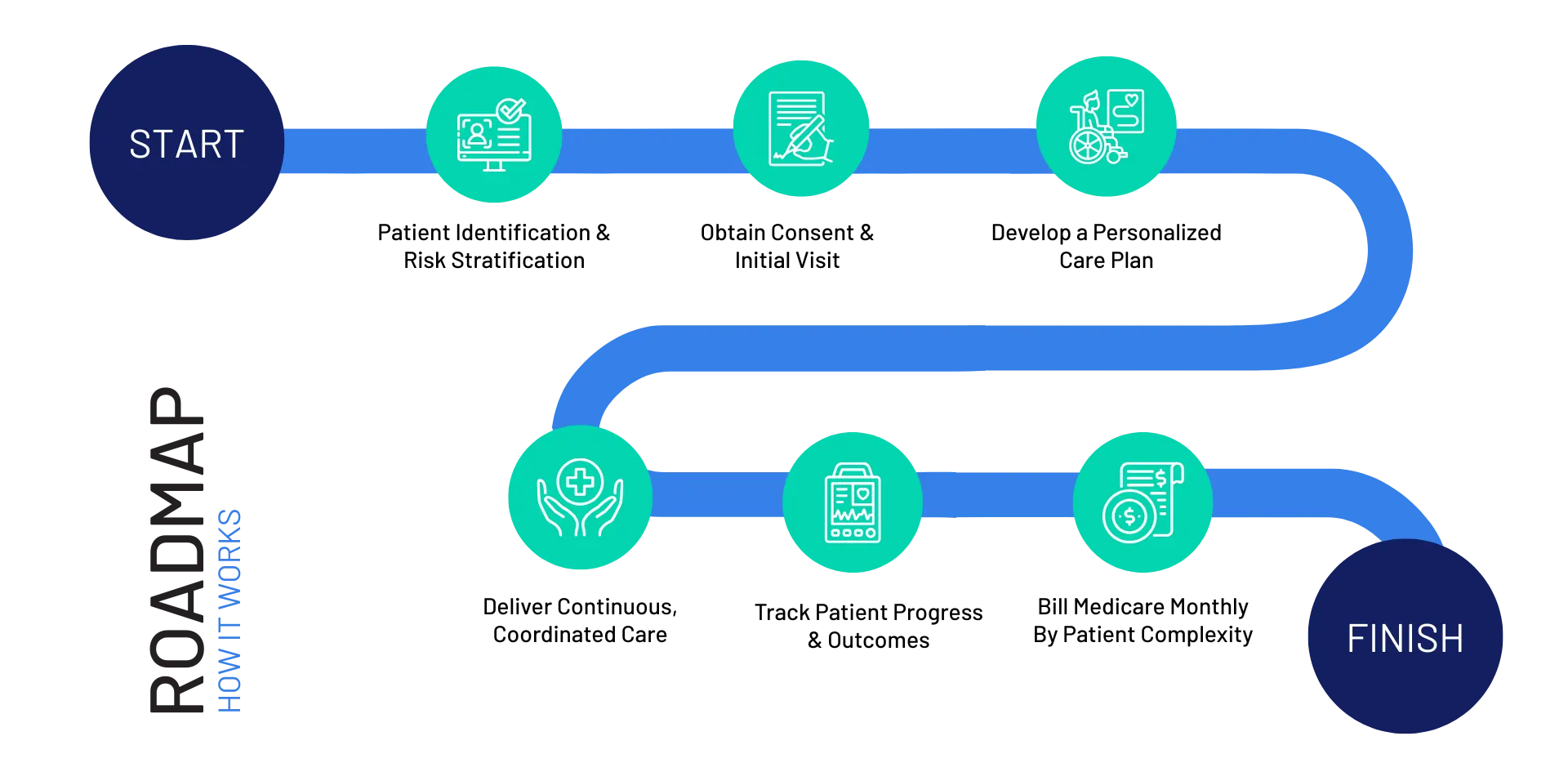
Request a Demo
CPT Billing Codes and Reimbursement for APCM
G0556 (GPCM1)
Patients with one or no chronic illness
$15.20
Medicare National Payment Amount (2025)
G0557 (GPCM2)
Patients with two or more chronic conditions (lasting ≥ 12 months)
$48.84
Medicare National Payment Amount (2025)
G0558 (GPCM3)
Qualified Medicare Beneficiaries (QMBs) meeting GPCM2 criteria
$107.07
Medicare National Payment Amount (2025)
Frequently Asked Questions
What is Advanced Primary Care Management (APCM)?
How APCM Differs from Existing Medicare Care Management Programs?
The proposed Advanced Primary Care Management (APCM) program introduces several key distinctions:
1. Three Risk-Based Billing Levels
APCM introduces three new billing codes aligned with different patient risk levels. Patients are stratified and enrolled in the level best suited to their care needs.
2. Activity-Based, Not Time-Based
Unlike prior programs, APCM reimbursement is based on completed care management activities rather than time spent. The monthly per-patient payment covers all qualifying services with no minimum time requirement.
3. Broader Patient Eligibility
APCM is open to all Medicare beneficiaries, including those with one or even no chronic conditions, greatly expanding participation beyond traditional chronic care programs.
4. Emphasis on Quality and Value
The program mandates quality measurement and reporting, reinforcing CMS’s commitment to value-based care and improved health outcomes.
When Will APCM Go Into Effect and How Will It Impact CCM and PCM Participants?
If finalized under the 2025 Medicare Physician Fee Schedule Proposed Rule, the Advanced Primary Care Management (APCM) program will take effect on January 1, 2025.
Practices currently participating in Chronic Care Management (CCM) or Principal Care Management (PCM) may also join APCM. However, each patient can only be enrolled in one monthly care management program at a time. Therefore, patients already participating in CCM or PCM would need to be re-enrolled under APCM to transition to the new model.
Resources
Wellwink Resources
Our Latest Blogs
Read the latest insights about Wellwink as well as medical blogs around the world. Our purpose is to provide education for both providers and patients.
Finding a Physician
Find a Physician and Book an Office visit or Virtual visit. We are helping healthcare communities to bridge the gap between patients and doctors.
